Dealing with digestive health issues can be uncomfortable and confusing. If you feel something unusual in your lower body, you are not alone. This guide, featuring insights from Dr. Jayadatt Pawar, the Best Colorectal Surgeon in New Delhi, will help you understand rectal prolapse clearly.
Dr. Jayadatt Pawar has 15+ years of experience and is a prestigious Bursary Award winner – AMASICON 2022. As a specialist in Gastrointestinal and Colorectal Disorders, he provides expert care for patients dealing with complex bowel issues.
What is Rectal Prolapse?
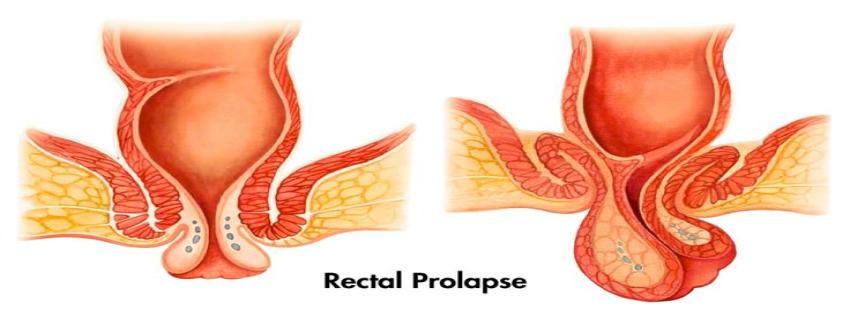
To understand what is rectal prolapse, we must first look at the rectum in the human body. The rectum is the last part of the large intestine that stores stool before it leaves the body.
In a prolapse meaning medical context, “prolapse” refers to a body part slipping out of its normal position. Therefore, the rectal prolapse meaning is when the rectum loses its attachment inside the body and slides down, sometimes poking out through the anus. This condition is common in rectal prolapse in adults and can also be seen as rectal prolapse in females due to pelvic floor changes.
Types of Rectal Prolap:
Not all cases are the same. Dr. Jayadatt Pawar explains that there are three main types:
- Internal Rectal Prolapse: In this stage, the rectum has started to slide but stays inside the body. It does not poke out of the anus yet. It is often hard to notice without a medical exam.
- External Rectal Prolapse: This is the most obvious type. The entire thickness of the rectal wall sticks out through the anal opening. Patients often describe it as hanging out tissue from anus.
- Mucosal Prolapse: Only the lining (mucosa) of the rectum slides down. This is common in children or people with long-term constipation problems.
Rectal Prolapse Symptoms:
Recognizing the signs early is vital. If you notice any of these rectal prolapse symptoms, you should consult a specialist:
- A lump in my back passage: Feeling a soft mass during or after a bowel movement.
- Bulging out of anus: Seeing reddish-pink tissue protruding outside.
- Something coming out of anus: This may happen while straining or even while walking.
- Mucus discharge from anus: You might see white discharge on poop or clear slime.
- Stool leakage: An inability to control bowel movements (incontinence).
- Incomplete bowel movement: Feeling like you haven’t finished your business.
- Pink stool: Mild bleeding can make the stool look pink or bright red.
Causes of Rectal Prolapse:
Why does this happen? Rectal prolapse causes usually involve a weakening of the muscles and ligaments that hold the rectum in place.
- Can constipation cause rectal prolapse? Chronic constipation leads to heavy straining, which pushes the rectum out over time.
- Weak pelvic muscles: Muscles can weaken due to surgery, childbirth, or age.
- Nerve damage: If the nerves controlling the rectal muscles are hurt, a prolapse can occur.
Risk Factors for Rectal Prolapse:
Certain factors increase your chances of developing this condition:
- Aging: Muscles naturally lose strength as we get older.
- Chronic Straining: Long-term coughing or lifting heavy weights.
- Pelvic Floor Disorders: Common in women who have had multiple vaginal births.
- Long-term Diarrhea: Frequent bathroom visits can put stress on the area.
Difference Between Rectal Prolapse and Hemorrhoids:
Many people confuse a prolapse with piles (hemorrhoids).
- Hemorrhoids: These are swollen blood vessels near the anal opening. They are usually smaller.
- Rectal Prolapse: This involves the actual rectal wall sliding down. It usually looks like a larger, circular ring of tissue.
When to See a Doctor:
You should not ignore rectal prolapse warning signs. According to Dr. Jayadatt Pawar, you should seek medical help if:
- The protrusion does not go back inside on its own.
- You experience severe pain or heavy bleeding.
- You have total loss of bowel control.
- You see severe rectal prolapse symptoms like tissue turning dark (loss of blood supply).
Diagnosis of Rectal Prolapse:
A rectal prolapse diagnosis starts with a simple conversation about your symptoms.
- Rectal Exam: The doctor will check the area visually.
- PR Exam (Per Rectal): Jayadatt Pawar will perform a gentle digital exam to check muscle strength.
- Defecography: An X-ray or MRI taken while you are having a bowel movement to see how the rectum functions.
Rectal Prolapse Treatment Options:
Many patients ask how to treat rectal prolapse without surgery.
- Rectal prolapse treatment without surgery: This works for very mild cases. It involves stool softeners, a high-fiber diet, and pelvic floor exercises (Kegels) to strengthen the muscles.
- Managing Constipation: Drinking plenty of water and eating fruits helps reduce straining.
However, for most adults, rectal prolapse treatment usually requires a surgical fix to secure the rectum back in place.
Common Surgical Procedures:
Rectal prolapse surgery is the most effective long-term solution. Dr. Jayadatt Pawar specializes in these advanced procedures:
- Rectopexy: This is a surgery where the rectum is pulled back up and stitched to the sacrum (bone at the base of the spine). It is often done laparoscopically (keyhole surgery).
- Altemier Procedure: The surgeon removes the prolapsed part of the rectum through the anus. This is often better for elderly patients who cannot handle abdominal surgery.
- Thiersch Wiring: A temporary fix where a ring is placed around the anus to keep the rectum inside.
Complications of Rectal Prolapse:
If left untreated, untreated rectal prolapse can lead to:
- Strangulation: The blood supply to the rectum gets cut off, causing tissue death.
- Ulcers: The protruding tissue can bleed or develop sores.
- Permanent Incontinence: Chronic stretching of the anal sphincter can lead to permanent stool leakage.
Rectal Prolapse Prevention Tips:
To prevent rectal prolapse, you must focus on healthy bowel habits:
- Avoid Constipation: Eat at least 25–30 grams of fiber daily.
- Hydrate: Drink 8–10 glasses of water.
- Don’t Strain: If the stool doesn’t come, don’t force it.
- Exercise: Keep your core and pelvic muscles strong.
- Listen to your body: Go to the washroom as soon as you feel the urge.
Conclusion:
Rectal prolapse is a treatable condition. You do not have to live with the discomfort or embarrassment of hanging out tissue from anus or mucus discharge from anus.
If you are looking for the best care, consult Dr. Jayadatt Pawar in New Delhi. With his vast experience in Colorectal Disorders, he can help you return to a comfortable and healthy life. Early diagnosis is the key to a quick recovery!
FAQS on Rectal prolapse:
While occasional constipation is common, chronic (long-term) constipation can lead to serious health issues if ignored. It is dangerous because:
- Straining: Constant pushing can cause rectal prolapse or painful hemorrhoids.
- Anal Fissures: Hard stools can tear the lining of the anus.
- Fecal Impaction: Stool can become so hard and stuck that it cannot be passed naturally.
- Toxins: It prevents your body from clearing waste effectively, leading to bloating and severe discomfort.
Dr. Jayadatt Pawar notes that women are statistically more likely to experience this condition. The primary causes include:
- Pregnancy and Childbirth: Multiple vaginal deliveries can weaken the pelvic floor muscles.
- Menopause: A drop in estrogen levels can lead to a loss of tissue strength in the pelvic region.
- Hysterectomy: Previous pelvic surgeries can sometimes disturb the support structures of the rectum.
- Chronic Straining: Long-term constipation problems over many years.
Non-surgical treatments focus on managing symptoms and preventing the prolapse from getting worse. You can try:
- Fiber-Rich Diet: Eat more green vegetables, fruits, and whole grains.
- Pelvic Floor Exercises: Doing “Kegels” helps strengthen the muscles supporting the rectum.
- Stool Softeners: Using over-the-counter softeners to avoid any straining.
- Hydration: Drink plenty of water to keep stools soft.
- Note: While these help mild cases (mucosal prolapse), Dr. Jayadatt Pawar advises that complete external prolapse usually requires a medical procedure for a permanent cure.
If the tissue has come out, you can sometimes gently push it back in, but you must be very careful:
- Be Gentle: Use a soft, lubricated cloth or disposable glove.
- Position: Lie down on your side or move into a “knee-to-chest” position to make it easier.
- Apply Pressure: Apply firm but very gentle upward pressure to ease the tissue back through the anal opening.
- Warning: If the tissue is stuck, painful, or turning a dark color, do not force it. Seek emergency medical help immediately.
You should book a consultation if you notice any of the following rectal prolapse warning signs:
- You feel a permanent lump in your back passage.
- You experience frequent stool leakage or an inability to control gas.
- There is significant bleeding or mucus discharge from the anus.
- The prolapsed tissue does not stay inside after being pushed back.
In older adults, the symptoms may be more pronounced due to naturally weaker muscles. Common signs include:
- Hanging out tissue from anus while walking or standing.
- Frequent “accidents” or bowel incontinence.
- A constant feeling of fullness or an incomplete bowel movement.
- Skin irritation and itching around the anal area due to constant moisture or mucus.